If you get dry eyes, checkout these fantastic tips on how to treat the condition. For more information check with the experts at Kirk Eye Center — see all that you can.
Exciting New Procedure to Remove Cataracts Quickly

If you have been recently diagnosed with cataracts, you may be interested in knowing there’s a new way to remove cataracts more quickly and speed up recovery time.
Dr. Sean Ianchulev, M.D. MPH, Professor or Ophthalmology at Icahn School of Medicine at Mount Sinai has created a device called the “miLOOP™.” It’s a simple device for microinterventional cataract surgery and used an “actuator,” (shaped like a pen) to enable “rapid non-thermal cutting of even the hardest cataracts without using laser, heat, or vibrational energy, with no fluidic complications.”
In layman’s terms, it’s a super quick way to remove cataracts and restore vision within a day or two of the procedure with little risk of complication. The exciting new procedure provides the fastest patient recovery time in cataract surgery history, and patients can see and read on the first day after the procedure.
What Are Cataracts?
Approximately 22 million Americans over the age of 40 have cataracts, and it is one of the leading causes of blindness. A cataract is a clouding of the normally clear lens of the eye, and people who have cataracts liken the condition to looking through a foggy window. Cataracts make activities of daily living like reading and driving more difficult and even impossible for many.
There are several different types of cataracts: cortical, nuclear, or subcapsular, but all cataracts cause blurry vision, and they may make lights seem too bright or glaring. Nighttime driving is especially difficult because of the glare of oncoming headlights and other lights around you. Colors may also not appear as bright as they once did after cataracts develop.
The lens of your eye is mostly made of water and protein with the protein being arranged to keep the lens clear and allow light to pass through. However, age causes some of this protein to clump together, and that’s when cataracts can occur. Most cataracts develop slowly and take years to affect your vision. What may not be a serious cataracts problem now will become more serious later as the cataracts affect your vision more and more.
According to the Mayo Clinic online, “[A]t first, the cloudiness in your vision caused by a cataract may affect only a small part of the eye’s lens and you may be unaware of any vision loss. As the cataract grows larger, it clouds more of your lens and distorts the light passing through the lens.”
A Bright Future for Cataract Sufferers
If you are over forty and don’t have cataracts, there is a very good chance you may develop this condition at a later time. The prevalence of cataracts in the United States is expected to grow significantly in the years ahead, due in part to the aging of the population. In 2010, roughly 24.4 million Americans had cataracts, and that number is projected to grow to 50.2 million by the year 2050, according to the National Eye Institute.
People having cataract surgery prior to the miLOOP™ had their cloudy lens replaced with an artificial lens known as an “IOL” (intraocular lens). Prior to insertion of the IOL, your ophthalmologist uses a high-frequency ultrasound device to break up the cloudy lens into small pieces; the pieces are then gently removed from the eye with suction in a procedure called “phacoemulsification”. After all remnants of the cloudy lens have been removed from your eye, the ophthalmologist inserts an IOL, positioning it securely behind iris and pupil, in the same location as your natural lens.
Because of its cost effectiveness and portability, the miLoop™ may provide first-world outcomes in third-world settings. It allows ophthalmologists to remove cataracts in areas they may not have access to the expensive technology necessary to perform other cataract procedures.
All About Tears – What You Need to Know
 TearT
TearT
We often only think of tears as associated with our emotions. However, tears play various important roles. Tears are essential for sight. They help to maintain healthy eyes. The average human produces an average of 30 gallons of tears annually. The following are some facts you should know about tears.
There is more than one type of tear
Humans produce three types of tears:
1- Emotional tears
These tears are trigged by strong emotional states such as joy, fear or sadness. These tears are thought to contain additional hormones and proteins that do not occur in other types of tears. Emotional tears have also been shown to have higher levels of manganese, prolactin, adrenocorticotropic hormone and potassium. The production of these tears is influenced by psychological, social and biological factors.
2- Reflex tears
These are formed as a defense against foreign bodies or harmful irritants e.g. smoke and onion fumes. These tears contain a larger volume of antibodies that are useful in fighting infections.
3 – Basal tears
These are produced for the primary purpose of lubricating the eye. They provide nourishment and protection to the cornea. They are a constant shield to the eye, keeping dirt and other contaminants off the eye surface.
The layers of tears
Tears are much more than a simple liquid. They contain lipids, enzyme, electrolytes and metabolites and have a structure that is similar to saliva. The following are the three layers of tears:
- Oily layer
This is the outer layer. It is important for preventing the inner layers from evaporating too quickly. It also keeps the surface of the tears smooth.
- Watery layer
This is the middle layer. It is also the thickest layer. It is important for keeping the eye’s surface moist. It is also important for repelling bacteria and protecting the cornea.
- Mucus layer
This is the innermost layer. It helps to adhere the tears to the surface of the eye.
Tears through the ages
Tear production reduces as we age. Production of basal tears slows down as we age leading to the development of dry eye. It is important to talk to an ophthalmologist to find out what you can do to protect your eyes and keep them moist. This may include using prescription eye drops, ointments or undergoing procedures to help improve tear production. Regular comprehensive eye exams will help to detect problems in their early stages.
Blepharitis – Causes, Symptoms and Treatment
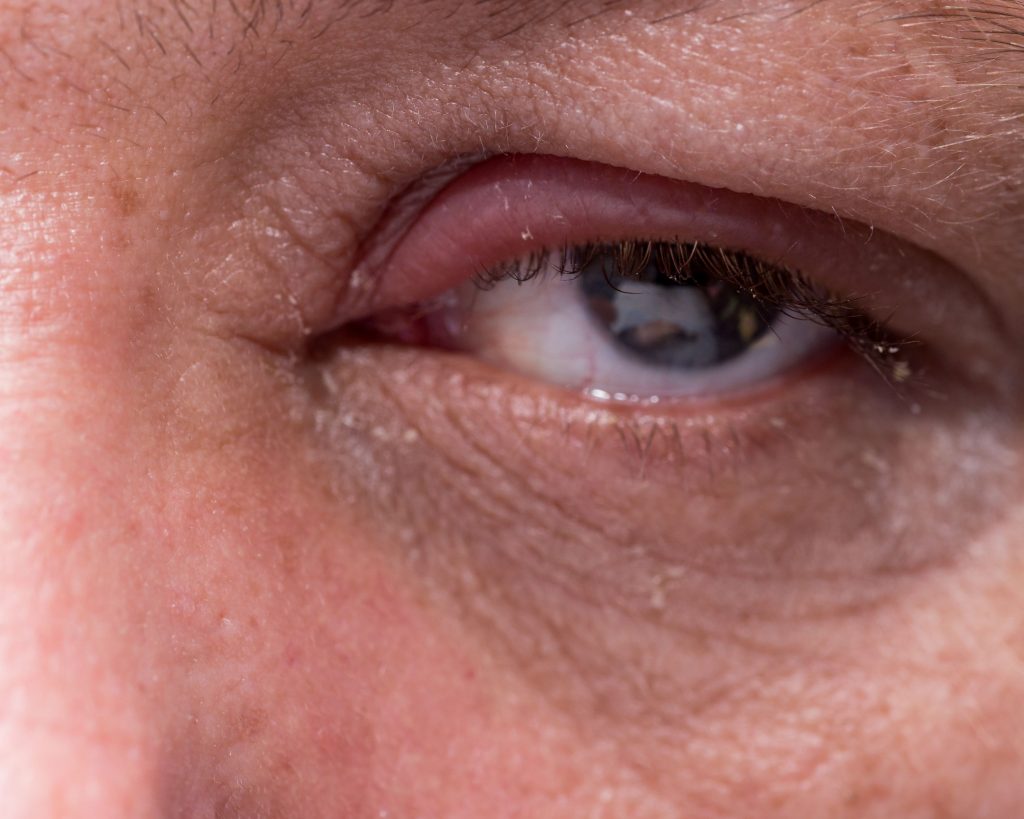
Blepharitis is a bacterial infection of the skin at the base of the eyelashes. The eyelids become red and swollen as a result. Oily flakes are formed on the eyelashes and there is a burning sensation on the eyelids.
Blepharitis is common especially amongst people with dry eyes, oily skin or dandruff.
Causes
Blepharitis results from the occurrence of a high number of bacteria on the skin at the base of the eyelashes. This results in the formation of flakes that appear like dandruff on the eyelashes. In some cases, the oil glands under the eyelids are also affected.
Treatment
There is currently no known cure for blepharitis. However, there are several things you can do to help in the management of the symptoms.
1- Apply warm compresses
Use a clean washcloth for this. Wet the cloth in warm water and wring it out. Close your eyes and place the cloth on them. Ensure that the cloth remains wet by continually wetting it and wringing out the warm water. Maintain this for at least 1 minute. This will help to loosen flakes and open up the clogged oil glands.
2- Make use of eyelid scrubs
Gently scrub the base of the eyelashes with a clean washcloth, lint-free pad or cotton swab dipped in warm water. Scrub your eyelids for at least 15 seconds at a time. This helps to get rid of flakes.
3 – Get eye drops
If you’re experiencing swelling, dry eyes and redness, antibiotic eye drops may help provide you with relief. Ask your ophthalmologist about the possibility of getting a prescription. Antibiotic eye drops will help the oil glands to function properly.
4 – Antibiotics
Antibiotic ointments can help to clear infections. Your ophthalmologist may prescribe an ointment that you can apply on your eyelids using a cotton swab. Your doctor may also prescribe an oral antibiotic to help clear infections.
5 – Practice hygiene
Keeping your hair, eyelids and skin clean goes a long way in managing blepharitis. Wash your eyelashes carefully every day. You can use a baby shampoo to enhance the cleaning without being harsh on the eyes. You may also use an antibacterial shampoo on your scalp, eyebrows and hair.
Antibacterial sprays may also be used to control the growth of bacteria on the skin. Use a facial moisturizer after cleaning your face to help keep your dry eyelids moisturized. Check with your ophthalmologist for more on helpful products.
Cataract Surgery – What Happens When the Results are Poor

While you can hope for the best results in a surgery, there are times when the results of a procedure aren’t as good as everyone hoped. If you’re anticipating a cataract surgery, you may be wondering what can be done in case you are not happy with the results of the surgery.
To answer this question, you will need to understand what is involved in a cataract surgery.
Cataract surgery
Cataract surgery is a permanent solution for cataracts. It involves the removal of the affected lens. The lens may then be replaced with an artificial lens. The artificial lens used to replace the natural lens will have been agreed upon before the procedure is undertaken.
By removing the entire lens and replacing it with an intraocular lens, the surgeon is able to improve the patient’s vision. It is rare that any complications occur from cataract surgery. The success rate of these surgeries is as high as 98%.
While complications are rare, possible complications from cataract surgery include:
- Macular edema – this is the swelling of the central part of the retina
- Ocular hypertension – this is the increase in pressure within the eye
- Light sensitivity
- Intraocular lens dislocation
- Eye inflammation
- Ptosis – the development of a droopy eyelid
- Photopsia – this is the perceived flashes of light in your field of vision
When these complications occur, they can often be solved medically. Some may require additional surgery.
Can I have an intraocular implant exchanged?
Intraocular lenses (IOLs) are designed to provide a permanent replacement for natural lenses that are removed during cataract surgery. There are a wide variety of IOLs at different magnification powers. These lenses function differently and have their advantages and disadvantages. Your surgeon will help you choose the most ideal solution for your needs.
The selection of an IOL takes time and care. This ensures that the right IOL is chosen. If the IOL implant does not provide the ideal power or is not properly positioned, it may be replaced or repositioned. It is however important for patients to realize that there are many risks involved in the replacement of IOLs.
There are various alternatives to exchanging an IOL. These include:
- Wearing prescription glasses
- Limbal relaxing incisions
- Wearing prescription contact lenses
- Laser vision correction.
If you’re considering an IOL exchange, it is important to consult with your surgeon and consider the pros and cons of the surgery.


